Notes: The following information is intended for health care professionals. Always read the label and follow the instructions for use. For information on the efficacy and the side effects, refer to the instructions for use. Products are only for sale to health professionals.
What are Anatomical Landmarks?
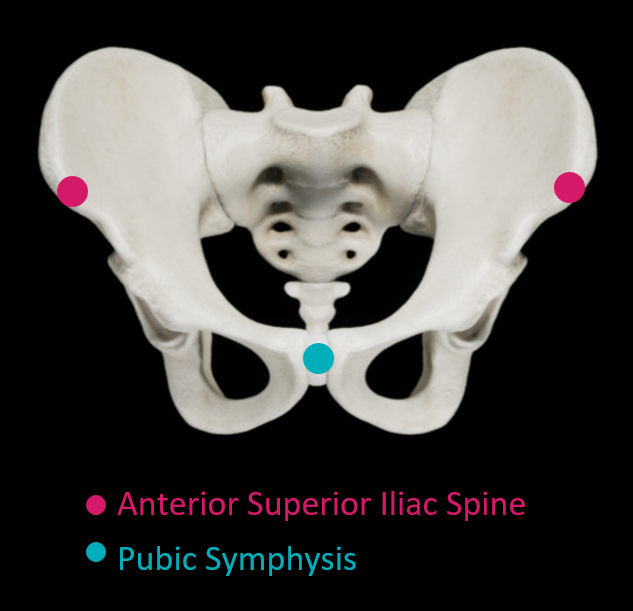
Many navigation systems require the surgeon to locate bony landmarks during patient registration. With navigation systems that use an anterior pelvic plane (APP) reference plane, surgeons generally palpate three bony landmarks: the anterosuperior iliac spines (ASISs) and the pubic symphysis1-6.
Why Does the Accurate Location of Landmarks Matter?
Accurate navigation relies on accurately registering a reference plane. Therefore, errors in locating bony landmarks translate into errors in navigation, which then lead to errors in component position.
What Causes Landmarking Errors?
Locating anatomical landmarks can be hindered by layers of surgical draping and the patient’s skin and soft tissue7. Small errors in landmark location lead to substantial errors in cup position: in a simulation that incorporated all rotational errors, a 4mm error in measuring each of the landmarks led to measurement errors of 2° for inclination and 7° for anteversion8. This higher error for anteversion is consistent with a cadaver study involving 8 surgeons, where the significant variation in measurement between surgeons (p < 0.001) resulted in significantly larger variation in anteversion (SD = 9.6°) than in inclination (SD = 6.3°)9. The distribution of soft tissue may contribute to these anteversion errors: the thickness of soft tissue was found to be greater over the pubic symphysis than over the ASISs by 5.7 ± 3.4 mm and to result in an anteversion error of -2.8° ± 1.8°10.
When are the Errors Worse?
Locating landmarks is particularly difficult with obese patients, leading to significantly higher errors7, 11, 12. For example, one study found a poor correlation between navigation measurements and post-operative acetabular inclination and anteversion in patients with a body-mass index (BMI) of at least 2713. A BMI of 27 is in the pre-obese range14. Other researchers found that inclination errors correlated positively with soft tissue thickness over the ASISs (r = 0.44; p = 0.007), and anteversion errors correlated positively with soft tissue thickness over the pubic symphysis (r = 0.52; p = 0.001)15. During robot-guided surgery with rigid patient positioning, anteversion errors were found to be significantly higher for the 50% of patients with a BMI above 27.516. According to these findings, as the amount of soft tissue increases, so do the errors.
These errors in landmarking due to soft tissue and obesity are consistent with reported surgical outcomes. Barrack, et al.17 found that the odds of a cup position outside of the target range increased as BMI increased17. Similarly, in Australian joint registry data, patients in the underweight, normal, and pre-obese BMI classes did not significantly differ, but patients in the obese class 1, obese class 2, and obese class 3 had significantly higher rates of revision14. With nearly three quarters of Australian THA patients either pre-obese or obese14, landmarking errors associated with soft tissue may be a substantial clinical problem.
What is the Solution?
One way to remove the errors associated with palpating bony landmarks is to develop patient registration methods that do not rely on locating these landmarks.
References
- Gurgel HMCP, Croci ATP, Cabrita HABAP, et al. Acetabular Component Positioning in Total Hip Arthroplasty With and Without a Computer-Assisted System – A Prospective, Randomized and Controlled Study. J Arthroplasty 2014;29(1):167-71. doi: 10.1016/j.arth.2013.04.017
- Davis ET, Schubert M, Wegner M, et al. A new method of registration in navigated hip arthroplasty without the need to register the anterior pelvic plane. J Arthroplasty 2015;30(1):55-60. doi: 10.1016/j.arth.2014.08.026 [published Online First: 2014/10/15]
- Lass R, Kubista B, Olischar B, et al. Total Hip Arthroplasty Using Imageless Computer-Assisted Hip Navigation A Prospective Randomized Study. J Arthroplasty 2014;29(4):786-91. doi: 10.1016/j.arth.2013.08.020
- Sendtner E, Schuster T, Wörner M, et al. Accuracy of acetabular cup placement in computer-assisted, minimally-invasive THR in a lateral decubitus position. Int Orthop 2011;35(6):809-15. doi: 10.1007/s00264-010-1042-4
- Cross MB, Schwarzkopf R, Miller TT, et al. Improving registration accuracy during total hip arthroplasty: a cadaver study of a new, 3-D mini-optical navigation system. Hip Int 2018;28(1):33-39. doi: 10.5301/hipint.5000533
- Wan Z, Malik A, Jaramaz B, et al. Imaging and Navigation Measurement of Acetabular Component Position in THA. Clin Orthop Relat Res 2009;467(1):32-42. doi: 10.1007/s11999-008-0597-5
- Lin FD, Lim DP, Wixson RLMD, et al. Limitations of Imageless Computer-Assisted Navigation for Total Hip Arthroplasty. J Arthroplasty 2011;26(4):596-605. doi: 10.1016/j.arth.2010.05.027
- Wolf A, Digioia AM, 3rd, Mor AB, et al. Cup alignment error model for total hip arthroplasty. Clin Orthop Relat Res 2005(437):132-7. doi: 10.1097/01.blo.0000164027.06880.3a
- Spencer JM, Day RE, Sloan KE, et al. Computer navigation of the acetabular component: a cadaver reliability study. J Bone Joint Surg Br 2006;88(7):972-5. doi: 10.1302/0301-620x.88b7.17468
- Richolt JA, Effenberger H, Rittmeister ME. How does soft tissue distribution affect anteversion accuracy of the palpation procedure in image-free acetabular cup navigation? An ultrasonographic assessment. Comput Aided Surg 2005;10(2):87-92. doi: 10.3109/10929080500229447
- Davenport D, Kavarthapu V. Computer navigation of the acetabular component in total hip arthroplasty: a narrative review. EFORT Open Rev 2016;1(7):279-85. doi: 10.1302/2058-5241.1.000050
- Feng JE, Anoushiravani AA, Eftekhary N, et al. Techniques for Optimizing Acetabular Component Positioning in Total Hip Arthroplasty: Defining a Patient-Specific Functional Safe Zone. JBJS Rev 2019;7(2):e5. doi: 10.2106/jbjs.Rvw.18.00049
- Parratte S, Argenson JN. Validation and usefulness of a computer-assisted cup-positioning system in total hip arthroplasty. A prospective, randomized, controlled study. J Bone Joint Surg Am 2007;89(3):494-9. doi: 10.2106/jbjs.F.00529
- Australian Orthopaedic Association National Joint Replacement Registry (AOANJRR). Hip, Knee & Shoulder Arthroplasty: 2021 Annual Report, 2021.
- Ybinger T, Kumpan W, Hoffart HE, et al. Accuracy of Navigation-Assisted Acetabular Component Positioning Studied by Computed Tomography Measurements: Methods and Results. The Journal of Arthroplasty 2007;22(6):812-17. doi: https://doi.org/10.1016/j.arth.2006.10.001
- Milone MTMD, Schwarzkopf RMDM, Meere PAMD, et al. Rigid Patient Positioning is Unreliable in Total Hip Arthroplasty. J Arthroplasty 2017;32(6):1890-93. doi: 10.1016/j.arth.2016.12.038
- Barrack RL, Krempec JA, Clohisy JC, et al. Accuracy of acetabular component position in hip arthroplasty. J Bone Jt Surg (Am) 2013;95(19):1760-8. doi: 10.2106/jbjs.L.01704 [published Online First: 2013/10/04]